The Gladstone Center for Translational Advancement was formed in 2017, and focuses on drug repositioning; repurposing already-approved drugs for new uses and clinical trials, to speed up (and lower the cost of) drug development.
Our neurologist reader Eszter
commented recently on the overlap between experimental therapies for
Alzheimer’s and those for autism. She was mentioning GHK-Cu, which is a naturally occurring peptide in our
bodies that looks interesting in the research on both Alzheimer’s and Parkinson’s. There will be post on GHK-Cu, but this is a
potential therapy that would require injections, so it has a big drawback
In the early days of this blog we
looked at the repurposing of Alzheimer’s drugs like Memantine, Donepezil and
Galantamine for some autism.
Roll forward a few years and we now have
quite a handful of autism drugs in the portfolio. Today we look again at how
some of these autism drugs can be repurposed for Alzheimer’s.
We have come full circle.
In a previous post we saw that
Fenamate NSAIDs, like Ponstan, reduce the incidence of Alzheimer’s. Only a low dose seems to be required for Alzheimer's and this
drug is extremely cheap in countries like Greece. A low dose seems to have a broad effect on autism. All in all very interesting, I believe.
We saw that Agmatine improves cognitive
dysfunction and prevents cell death in a Streptozotocin-Induced Alzheimer rat model.
We saw that the ketone BHB
inhibits inflammasome activation to attenuate Alzheimer's disease pathology.
I have mentioned the interest to repurpose Verapamil to
treat Huntington’s disease, via its effect on autophagy, but there is also
interest to use it in Alzheimer’s.
Repurposing verapamil for prevention of cognitive decline in sporadic Alzheimer’s disease
Today we will look at why Bumetanide and Clemastine may be beneficial in Alzheimer’s.
A quick summary of Alzheimer’s Disease
Alzheimer’s disease features
prominently plaques (amyloid plaques) and fibers (tau tangles) that are visible
within the brain.
It is
thought that inhibiting the aggregation and accumulation of amyloid
plaques and tau in the brain is the key to treating Alzheimer’s Disease.
We did see that that the red pigment
in beetroot has been shown to block the formation of amyloid plaques and no
prescription is required for that superfood.
In addition, we know that there is
reduced glucose uptake across the blood brain barrier via the GLUT1 and GLUT3
transporters. In effect the brain is
left starving. There is also impaired insulin signalling within the brain, this led to the idea of intranasal
insulin as a treatment. The insulin
dependent glucose transporter GLUT4 plays a central role in hippocampal memory
processes, and reduced activation of this transporter may underpin the
cognitive impairments seen in Alzheimer’s disease and more generally in those
who develop insulin resistance. (more insulin inside the brain, please)
We also
did look at the recently discovered lymphatic drainage system of the brain. It
was seen that this waste clearing system is impaired in Alzheimer’s and perhaps
some autism. This then takes us back to the autophagy process within the brain,
where cellular waste is collected. It is thought that autophagy itself is
impaired in autism. Collecting and disposing of brain garbage does not function
as it should.
Over a
decade or so, the brain gradually shrinks away and loses functions. I think in reality Alzheimer’s initially
develops slowly, years before diagnosis.
The
currently prescribed drugs do not alter the course of the disease and often
provide only minimal benefit. Donepezil increases acetylcholine concentrations at
cholinergic synapses and upregulates nicotinic receptors. Memantine blocks NMDA
receptors. Much more appears to be
possible.
This is an autism blog so let’s be aware of the research on the overlaps with Alzheimer’s.
Alzheimer’s protein turns up as potential target for autism treatments
Lowering the levels of a
protein called tau, best known for its involvement in Alzheimer’s disease,
eases autism-like traits in mice, according to a study published today in Neuron.
Tau regulates a gene
called PTEN, according to a 2017 study4. PTEN accounts for 2 to 5 percent of autism cases and is known to modulate the PI3K pathway; without it, the
pathway becomes overactive, in some cases leading to autism.
Mucke’s team found that knocking out PTEN in neurons blocks the effect of lowering tau on the mice’s behaviors.
Proteomics of autism and
Alzheimer’s mouse models reveal common alterations in mTOR signaling pathway
Certain genes can increase the risk of
developing dementia, including Alzheimer’s disease. One of the most significant
genetic risk factors is a form of the apolipoprotein E gene called APOE4. About
25% of people carry one copy of APOE4, and 2 to 3% carry two copies. APOE4 is
the strongest risk factor gene for Alzheimer’s disease, although inheriting
APOE4 does not mean a person will definitely develop the disease.
The APOE gene
comes in several different forms, or alleles. APOE3 is the most common and not believed to affect
Alzheimer’s risk. APOE2 is relatively rare and may provide some
protection against Alzheimer’s disease.
The reason APOE4 increases Alzheimer’s risk is not well
understood. The APOE protein helps carry cholesterol and other types of fat in
the bloodstream. Recent studies suggest that problems with brain cells’ ability
to process fats, or lipids, may play a key role in Alzheimer’s and related
diseases.
Regular readers
of this blog will be familiar of the remarkable effects of statin drugs. So
from the mention of cholesterol we take a brief diversion to see how people who
start taking statins before older age get yet another benefit.
"Additionally, statins could reduce dementia risk by directly
affecting Alzheimer’s disease pathology. A study in transgenic mice models of Alzheimer’s disease
found that atorvastatin reduced Aβ formation [69], and atorvastatin can attenuate some the damage from
neuroinflammation in Alzheimer’s disease
[70].
Much of the evidence supporting statins in the prevention of
dementia and AD are in persons exposed to statins at mid-life as opposed to
late life. This suggests that statins benefits may be limited to the vascular
prevention stage of AD and dementia. "
Back to Bumetanide.
The easy to read article:-
Can
an Already Approved Drug Treat Alzheimer’s Disease?
An Alternative Approach to Drug Discovery
Developing new,
targeted drugs for complex conditions like Alzheimer’s disease is a notoriously
long and expensive process. In 2017, with the goal of bringing safe treatments
to patients more quickly, Huang launched the Gladstone Center for Translational Advancement to repurpose FDA-approved drugs for new uses.
Huang’s approach
centers around the idea that patients with Alzheimer’s disease may have
different underlying causes of neurodegeneration, and therefore, the efficacy
of specific treatments may differ among patients—a strategy called precision
medicine. However, in the large clinical trials required for new drugs, it can
be hard to pinpoint whether a drug is effective in only a subpopulation of the
patients.
Therefore,
the research team used a computational approach to identify unique gene
expression profiles (or the level to which genes are turned on or off)
associated with Alzheimer’s disease in brain tissues from specific subgroups of
patients. They then screened a database of existing drugs to find the ones most
likely to reverse the altered gene expression profiles in each subgroup.
In the new study,
the researchers first analyzed a publicly available database of 213 brain
samples from people with and without Alzheimer’s disease, including people with
different versions of a gene called APOE, the major genetic risk factor for the disease.
The team identified
nearly 2,000 altered gene expressions in the brains of people with Alzheimer’s
disease. While roughly 6 percent of the altered genes were similar between
people with different APOE versions, the vast majority of them were unique
to people with specific combinations of the APOE3 or APOE4 versions,
the latter conferring the highest genetic risk of Alzheimer’s disease.
The researchers next
queried a database of more than 1,300 existing drugs to look for those able to
change the altered gene expressions they had identified for subgroups of
Alzheimer’s patients. They zeroed in on the top five drugs that might reverse
the altered gene expressions found in Alzheimer’s patients carrying two copies
of the high-risk APOE4 version.
“This unbiased
approach allowed us to find which drugs might be able to flip the altered gene
expression associated with APOE4-related Alzheimer’s disease back to the normal
state,” says Alice Taubes, PhD, lead author of the study and former graduate
student in Huang’s lab at Gladstone and co-mentored by Marina Sirota at UCSF.
“It gave us important clues in solving the puzzle of which drugs could be
effective against APOE4-related Alzheimer’s disease.”
After looking at the known mechanisms and previous data on
the drugs in their top-five list, the researchers homed in on bumetanide, a diuretic that reduces extra fluid in the body caused by
heart failure, liver disease, and kidney disease. Bumetanide is known to work
by changing how cells absorb sodium and chloride—both important not only for
maintaining appropriate levels of water throughout the body, but also for
electrical signaling of neurons in the brain.
Huang and his team
tested the effect of bumetanide on mice genetically engineered to have
human APOE genes.
Mice with two copies of the human APOE4 version typically develop learning and
memory deficits around 15 months of age—the equivalent of roughly 60 years in
humans. But when the researchers treated the mice with bumetanide, they no
longer developed such deficits. In addition, the drug rescued alterations in
electrical brain activity that can underlie these cognitive deficits.
The scientists also
studied a second mouse model of Alzheimer’s disease, in which two copies
of APOE4 coexist
with amyloid plaques—a major pathological sign of Alzheimer’s disease in the
brain. In these mice, bumetanide treatment decreased the number of amyloid
plaques and restored normal brain activity.
Lastly, when the
researchers studied the effect of the drug on human neurons derived from skin
cells of Alzheimer’s patients carrying the APOE4 gene, they
found that bumetanide reversed the gene expression changes associated with the
disease.
… the researchers evaluated two large electronic health
record databases—one from UCSF containing information on 1.3 million patients
seen from 2012 through 2019, and another from the Mount Sinai Health System
covering 3.9 million patients seen from 2003 through 2020. They narrowed in on
more than 3,700 patients who had taken bumetanide and were over the age of 65,
and compared them to patients of similar age and health who had taken different
diuretic drugs. Strikingly,
the patients who had taken bumetanide were 35 to 75 percent less likely to be
diagnosed with Alzheimer’s disease.
The full paper:-
It gets a bit heavy, so just skip
through it.
The evident genetic, pathological and clinical heterogeneity of Alzheimer’s disease (AD) poses challenges for traditional drug development. We conducted a computational drug-repurposing screen for drugs to treat apolipoprotein E4 (APOE4)-related AD. We first established APOE genotype-dependent transcriptomic signatures of AD by analyzing publicly available human brain databases. We then queried these signatures against the Connectivity Map database, which contains transcriptomic perturbations of more than 1,300 drugs, to identify those that best reverse APOE genotype-specific AD signatures. Bumetanide was identified as a top drug for APOE4-related AD. Treatment of APOE4-knock-in mice without or with amyloid β (Aβ) accumulation using bumetanide rescued electrophysiological, pathological or cognitive deficits. Single-nucleus RNA sequencing revealed transcriptomic reversal of AD signatures in specific cell types in these mice, a finding confirmed in APOE4 induced pluripotent stem cell (iPSC)-derived neurons. In humans, bumetanide exposure was associated with a significantly lower AD prevalence in individuals over the age of 65 years in two electronic health record databases, suggesting the effectiveness of bumetanide in preventing AD.
Bumetanide
exposure is associated with a significantly lower AD prevalence in individuals
over the age of 65. We hypothesized that, if bumetanide is efficacious against AD, we
would observe a lower prevalence of AD diagnosis in individuals exposed to
bumetanide than in a matched control cohort of individuals over the age of 65
years. To test this hypothesis in humans, we analyzed two independent EHR
databases (Fig. 7a). One is an EHR database from the University of California
at San Francisco (UCSF), which contains complete medical records for 1.3
million patients from outpatient, inpatient and emergency room encounters as
part of clinical operations from June 2012 to November 2019. The UCSF EHR
database was filtered using the medication order table for patients on the drug
of interest, and we found 5,526 patients who had used bumetanide (other names,
Bumex or Burinex). Among them, 1,850 patients (1,059 men (57.2%) and 791 women
(42.8%)) were over the age of 65. The other EHR database was from the Mount
Sinai Health
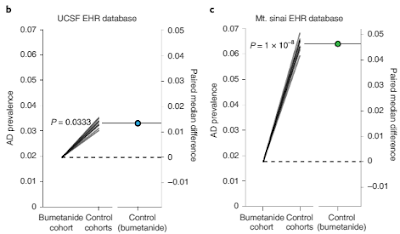
Fig. 7 | Bumetanide exposure is associated with a significantly lower AD prevalence in individuals over the age of 65 in two independent EHR databases.
Bootstrapped χ2 tests40 confirmed a significantly
lower AD prevalence in bumetanideexposed individuals than that in
non-bumetanide-exposed individuals in both EHR databases (Fig. 7b,c). Together, these data suggest that
bumetanide may be effective in preventing AD in individuals over the age of 65
years, warranting further tests in prospective human clinical trials.
Discussion
This study represents an attempt to apply a
precision medicine approach to computational drug repurposing for AD in an APOE
genotype-directed manner. The efficacy of a top predicted drug, bumetanide, for
APOE4 AD was validated in vivo in both aged APOE4-KI (without Aβ accumulation)
and J20/E4-KI (with Aβ accumulation) mouse models of AD for rescue of
electrophysiological, pathological or behavioral deficits. Importantly, by
leveraging real-world data, bumetanide exposure was associated with a significantly
lower AD prevalence in individuals over the age of 65 years in two independent
EHR databases, suggesting the potential effectiveness of bumetanide in
preventing AD in humans.
Bumetanide exposure is associated with a significantly lower AD prevalence in individuals over the age of 65 in two independent EHR databases.
Clemastine for Alzheimer’s
The research suggests multiple
possible benefits from the use of the cheap antihistamine Clemastine in
Alzheimer’s.
Clemastine
Attenuates AD-like Pathology in an AD Model Mouse via Enhancing mTOR-Mediated
Autophagy
Background: Alzheimer’s disease (AD) is a neurodegenerative disorder with limited available drugs for treatment. Enhancing autophagy attenuates AD pathology in various AD model mice. Thus, development of potential drugs enhancing autophagy may bring beneficial effects in AD therapy. Methods: In the present study, we showed clemastine, a first-generation histamine H1R antagonist and being originally marketed for the treatment of allergic rhinitis, ameliorates AD pathogenesis in APP/PS1 transgenic mice. Chronic treatment with clemastine orally reduced amyloid-β (Aβ) load, neuroinflammation and cognitive deficits of APP/PS1 transgenic mice as shown by immunohistochemistry and behavioral analysis. We further analyzed the mechanisms underlying the beneficial effects of clemastine with using the combination of both in vivo and in vitro experiments. We observed that clemastine decreased Aβ generation via reducing the levels of BACE1, CTFs of APP. Clemastine enhanced autophagy concomitant with a suppression of mTOR signaling. Conclusion: Therefore, we propose that clemastine attenuates AD pathology via enhancing mTORmediated autophagy.
Disrupted myelin and impaired myelin repair
have been observed in the brains of patients and various mouse models of
Alzheimer’s disease (AD). Clemastine, an H1-antihistamine, shows the capability
to induce oligodendrocyte precursor cell (OPC) differentiation and myelin
formation under different neuropathological conditions featuring
demyelination via the antagonism of M1 muscarinic receptor. In
this study, we investigated if aged APPSwe/PS1dE9 mice, a model of AD, can
benefit from chronic clemastine treatment. We found the treatment reduced brain
amyloid-beta deposition and rescued the short-term memory deficit of the mice.
The densities of OPCs, oligodendrocytes, and myelin were enhanced upon the
treatment, whereas the levels of degraded MBP were reduced, a marker for
degenerated myelin. In addition, we also suggest the role of clemastine in
preventing OPCs from entering the state of cellular senescence, which was shown
recently as an essential causal factor in AD pathogenesis. Thus, clemastine exhibits therapeutic
potential in AD via preventing senescence of OPCs.
Reversing Alzheimer's disease dementia with clemastine, fingolimod, or rolipram, plus anti‐amyloid therapy
A few anti‐amyloid trials offer a slight possibility of preventing progression of cognitive loss, but none has reversed the process. A possible reason is that amyloid may be necessary but insufficient in the pathogenesis of AD, and other causal factors may need addressing in addition to amyloid. It is argued here that drugs addressing myelination and synaptogenesis are the optimum partners for anti‐amyloid drugs, since there is much evidence that early in the process that leads to AD, both neural circuits and synaptic activity are dysfunctional. Evidence to support this argument is presented. Evidence is also presented that clemastine, fingolimod, and rolipram, benefit both myelination and synaptogenesis. It is suggested that a regimen that includes one of them plus an anti‐amyloid drug, could reverse AD.
Note that Rolipram is a selective PDE4 inhibitor that never made it to use in humans. Roflumilast is very similar and counts as an autism drug in this blog, alongside Pentoxifylline, which is a non-selective PDE inhibitor (if affects more than just PDE4).
Conclusion
It looks like if you were an
enlightened neurologist treating autism you would have the drugs needed to make
a fair crack at treating, or preventing, Alzheimer’s. Unfortunately, once they are established, you
are not going to cure either disease; nonetheless, fully treating autism will
carry forward the person further than their ABA therapist would ever have
dreamed possible. Treating Alzheimer's successfully will depend on when you start, best to start as soon as the signs appear on an MRI or CT scan, not a few years later.
Prevention is better than cure; indeed
an older person’s multipurpose Polypill looks to be in order. This could go beyond the usual cardiovascular concerns and include prevention/mitigation of dementia and diabetes (e.g. statin, low dose ponstan, verapamil and a mix of betanin, spermidine, agmatine with ALA or NAC)
Just because you might carry the APO4
gene does not mean you will develop Alzheimer’s, but it is a good reason to
take steps to prevent it.
There is a long list of factors that
increase the incidence/severity of autism, so there are is an equal number of
steps that can be taken to reduce it.
The gene expression study showed that
Bumetanide has wide ranging effects within the brain that counter the defects
found in APO4 mice and humans who have developed Alzheimer’s. This suggests that bumetanide’s effects go
well beyond blocking the NKCC1 cotransporter.
This may explain why some bumetanide responders with autism have a
paradoxical reaction to GABA agonists, like benzodiazepines, and some people do
not. They are receiving different beneficial effects.
We will look at the anti-inflammatory benefits of bumetanide suggested in very recent Chinese research in the next post. This might provide biomarkers for likely responders.
You might have thought that clemastine
would not be good for dementia, because it is anticholinergic, as are many
antihistamines and even drugs commonly given to older people like Nexium. The
neurotransmitter acetylcholine is good for cognition and it has been suggested
that depleting it might lead to dementia.
It looks like our off-label MS drugs,
clemastine, Ibudilast and Roflumilast are going to be good for dementia, not to
forget our new reader Bob and his Pentoxifylline.
It is notable that Gladstone Center for
Translational Advancement exists. There are clearly very many existing drugs that can be
repurposed to treat all kinds of medical issues. I keep discovering more, which
is good for me. Bob discovered Pentoxifylline, which is good for him and his
patients. Other people are free to make
their own choices.