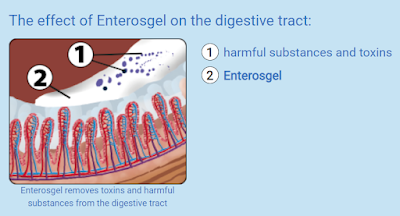
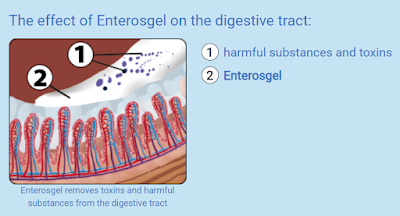
Today’s post has two themes, one relates to Transitory Autism, where a toddler with autism appears to “grow out” of the condition and the other is another substance produced in the gut, like we saw earlier with Propionic acid, that can produce “autism”.
Increased intestinal transit time and bacteria produce P-Cresol
If your gut produces a lot of propionic acid, instead of butyric acid, you can appear to have autism.
Today we see that producing too much P-Cresol in your gut produces symptoms of autism.
I suspect in most cases P-Cresol is making severe autism worse, rather than making a neurologically healthy, but likely constipated, person exhibit autism.
Elevated P-Cresol is associated with increased intestinal transit time and not Clostridium type bacteria. We know that elevated P-Cresol is reduced after oral supplementation with oligofructose-enriched inulin. It is suggested that certain probiotic bacteria might also lower P-Cresol. A microbiota transplant, from a healthy subject, reversed P-Cresol abnormalities in a mouse model.
Interestingly, elevated P-Cresol alters the microbiome in the gut, so there may be a vicious circle. An altered microbiome elevates P-Cresol and elevated P-Cresol produces an altered microbiome.
The Italian research on this subject suggests that in some people, resolving chronic constipation might solve most of the problem.
If your gut is producing toxic chemicals, it is not surprising that the studies using microbiota (fecal) transplants show transformative results in some children.
Fermentation in your Gut
Today it looks like we have another chemistry lesson.
We have come across all sorts of chemicals in this autism blog with all kinds of acronyms, like SCFA (short chained fatty acid).
You have all kinds of autism treatments, like Nemechek and his Propionic Acid (an SCFA) lowering protocol. We saw in an earlier post how injecting a mouse with propionic acid (PPA) makes it autistic and that giving it NAC returns the mouse to its original state. The Koreans have just moved this research forward and found what is happening in the brain. Propionic acid reduces the number of dendritic spines. See the lower right illustration.
Propionic Acid (PPA) decreases density of dendritic spines in hippocampal neurons
Propionic acid induces dendritic spine loss by MAPK/ERK signaling and dysregulation of autophagic flux
Propionic acid (PPA) is a short-chain fatty acid that is an important mediator of cellular metabolism. It is also a by-product of human gut enterobacteria and a common food preservative. A recent study found that rats administered with PPA showed autistic-like behaviors like restricted interest, impaired social behavior, and impaired reversal in a T-maze task. This study aimed to identify a link between PPA and autism phenotypes facilitated by signaling mechanisms in hippocampal neurons. Findings indicated autism-like pathogenesis associated with reduced dendritic spines in PPA-treated hippocampal neurons. To uncover the mechanisms underlying this loss, we evaluated autophagic flux, a functional readout of autophagy, using relevant biomedical markers. Results indicated that autophagic flux is impaired in PPA-treated hippocampal neurons. At a molecular level, the mitogen-activated protein kinase (MAPK)/extracellular signal-regulated kinase (ERK) pathway was activated and autophagic activity was impaired. We also observed that a MAPK inhibitor rescued dendritic spine loss in PPA-treated hippocampal neurons. Taken together, these results suggest a previously unknown link between PPA and autophagy in spine formation regulation in hippocampal neurons via MAPK/ERK signaling. Our results indicate that MAPK/ERK signaling participates in autism pathogenesis by autophagy disruption affecting dendritic spine density. This study may help to elucidate other mechanisms underlying autism and provide a potential strategy for treating ASD-associated pathology.
Fermentation
Fermentation in your colon, right now
In the graphic above you can see the types of chemicals that are produced in your gut by fermentation.
Fermentation is the chemical breakdown of a substance by bacteria, yeasts, or other microorganisms.
In the graphic you can see SCFA and BCFA. At the top right you can see Phenol.
I had never heard of P-Cresol, so I looked it up.
From high school chemistry many people may recall Benzene (C6H6). It is drawn as a ring.
· knock off an H and add an OH and you have Phenol.
In the top of the graphic about fermentation in your gut are phenol compounds.
If you start with phenol, knock off another H, add a CH3 (methyl radical) and you get P-Cresol CH3C6H4(OH).
A more helpful name they could have used in the research is methylphenol.
So now we know that if you ferment protein in your gut, certain bacteria will end up producing compounds related to phenol, one of which is P-cresol.
It looks like protein staying too long in the colon is a big part of the problem.
Other potential nasties in your gut
It is pretty clear that there will be numerous other chemicals produced in your gut that are not so good for you.
What about all that ammonia (NH3) produced in your colon?
You could write a book just about these potential gut nasties.
Back to P-Cresol
It turns out that high levels of P-Cresol can produce transitory autism.
The study below showed that:-
· you can make mice “autistic” by feeding them with P-Cresol
· The affected mice developed altered gut bacteria (microbiota)
· Transplanting the altered microbiota will make another mouse autistic
· Transplanting healthy microbiota to a P-cresol mouse reverses its autism
Background
Perturbations of the microbiota-gut-brain axis have been identified in autism spectrum disorders (ASD), suggesting that the microbiota could be involved in the development or maintenance of abnormal social and stereotyped behaviors in ASD patients. Yet, the underlying mediators and mechanisms remain unclear. We hypothesized that microbial metabolites produced by the gut microbiota contribute to behavioral deficits in ASD. We focused on p-Cresol, a microbial metabolite previously described as abnormally elevated in ASD patients.
Methods
Wild-type mice were chronically treated with p-Cresol in drinking water to mimic intestinal exposure. We combined behavioral phenotyping, electrophysiology, microbiota 16S sequencing and fecal microbiota transplantations to decipher the consequences of p-Cresol exposure.
Results
We showed that p-Cresol selectively induced behavioral alterations reminiscent of ASD core symptoms: social behavior deficits, stereotypies and perseverative behaviors, but no changes in anxiety, locomotion or cognition. We further showed that p-Cresol decreases the activity of dopamine neurons in the ventral tegmental area (VTA), a key brain region for social reward processing. In addition, we reveal that p-Cresol remodels the intestinal microbiome, impacting specific bacterial taxa associated with social behavior deficits and stereotypies. We further demonstrated that social behavior deficits are transferred to control mice after transplantation of microbiota from p-Cresol-treated mice. Finally, both social interactions and VTA dopamine neurons activity were normalized in p-Cresol treated mice after transplant of microbiota from control mice.
Conclusions
Our study suggests that the microbial metabolite p-Cresol could be involved in the development of autistic behaviors through remodeling of the gut microbiota.
How relevant is a P-Cresol mouse to a human toddler?
The research is distinctly Italian and we come across Dr Persico again.
It seems that P-Cresol is elevated in toddlers with severe autism, but not so much in older children with autism
If you lowered the level of P-cresol in these children you would likely reduce the severity of their autism.
Autism spectrum disorder (ASD) is a neuropsychiatric disorder with onset during early childhood and life-long consequences in most cases. It is characterized by impairment in social interaction and communication, as well as by restricted patterns of interest and stereotyped behaviors. The etiology of autism is highly heterogeneous, encompassing a large range of genetic and environmental factors. Several lines of evidence suggest that, in addition to broader diagnostic criteria and increased awareness, also a real increase in incidence primarily due to greater gene-environment interactions may also be occurring. Environmental exposure to the organic aromatic compound p-cresol (4-methylphenol) is relatively common and occurs through the skin, as well as the gastrointestinal and respiratory systems. However, the largest and most widespread source of this compound is represented by some gut bacteria which express p-cresol synthesizing enzymes not found in human cells. Urinary p-cresol and its conjugated derivative p-cresylsulfate have been found elevated in an initial sample and recently in a replica sample of autistic children below 8 years of age, where it is associated with female sex, greater clinical severity regardless of sex, and history of behavioral regression. Potential sources of p-cresol excess in ASD, such as gut infection, chronic constipation, antibiotics, abnormal intestinal permeability, and environmental exposure, are being investigated. P-cresol may contribute to worsen autism severity and gut dysfunction, often present in autistic children. It may also contribute to a multibiomarker diagnostic panel useful in small autistic children.
The results summarized in Section 3, spurred our interest into assessing urinary levels of p-cresol in 59 non-syndromic autistic children and in 59 tightly age- and sex-matched controls (Altieri et al., 2011). Urinary p-cresol was measured in first morning urines by high performance liquid chromatography-ultraviolet (HPLC-UV) with multi-wavelength diode array detector (DAD). Urinary concentrations of p-cresol were significantly higher in autistic children compared to controls (123.5± 12.8 vs. 91.2±8.7 μg/ml, Pb0.05). This elevation was surprisingly age-dependent, as it was clearly detectable only up until and including age 7 (134.1±20.1 vs. 70.3±6.7 μg/ml, P=0.005), with urinary p-cresol levels normalizing at age 8 and beyond. Levels of p-cresol were correlated neither with body mass index nor with urinary cotinine levels, excluding spurious contamination from passive smoking.
Instead, p-cresol levels were significantly higher among:
(a) female autistic children compared to males (Pb0.05);
(b) more severely affected autistic children, regardless of sex (Pb0.05);
(c) children who underwent regression at autism onset, based on parents reporting loss of language skills after acquisition of more than 5 spoken words and loss of social abilities after initial acquisition (Pb0.05).
The currently available evidence summarized in this review provides initial support for postnatal exposure to elevated p-cresol and/or p-cresylsulfate as a pathoplastic contributor to the severity of behavioral abnormalities and cognitive impairment in autistic children. In particular, p-cresol and/or p-cresylsulfate seemingly belong to a restricted set of gut- or environmentally-derived compounds potentially able to worsen behavioral abnormalities and cognitive impairment in small autistic children. Studies performed in specific cellular and animal models, as well as prospective follow-up studies involving baby siblings (i.e., “high-risk” neonates born to parents with one grown-up child already diagnosed with ASD) will be instrumental in determining whether early prenatal exposure to environment- or maternal gut derived p-cresol may provide pathogenic contributions, significantly increasing the risk of autism spectrum disorder in the offspring. It will also be important to determine the precise origin of elevated p-cresol in small autistic children and to define its influence on the spectrum and intensity of clinical signs and symptoms of ASD, on developmental trajectories, and on endophenotypic subgroupings of small children with ASD. Replication studies will also need to determine whether elevated urinary p-cresol/p-cresylsulfate in ASD is specific to some racial and ethnic groups or represents a generalized finding. If positive, these studies spur hope into the design of cresol-resistant probiotics possibly able to improve behavioral abnormalities when targeted to ASD children with elevated urinary p-cresol.
Several studies have described in autistic patients an overgrowth of unusual gut bacterial strains, able to push the fermentation of tyrosine up to the formation of p-cresol. We compared levels of urinary p-cresol, measured by high-performance liquid chromatography-ultraviolet, in 59 matched case-control pairs. Urinary p-cresol was significantly elevated in autistic children smaller than 8 years of age (p < 0.01), typically females (p < 0.05), and more severely affected regardless of sex (p < 0.05). Urinary cotinine measurements excluded smoking-related hydrocarbon contaminations as contributors to these differences. Hence, elevated urinary p-cresol may serve as a biomarker of autism liability in small children, especially females and more severely affected males.
The uremic toxin p-cresol (4-methylphenol) is either of environmental origin or can be synthetized from tyrosine by cresol-producing bacteria present in the gut lumen. Elevated p-cresol amounts have been previously found in the urines of Italian and French autism spectrum disorder (ASD) children up until 8 years of age, and may be associated with autism severity or with the intensity of abnormal behaviors. This study aims to investigate the mechanism producing elevated urinary p-cresol in ASD. Urinary p-cresol levels were thus measured by High Performance Liquid Chromatography in a sample of 53 Italian ASD children assessed for (a) presence of Clostridium spp. strains in the gut by means of an in vitro fecal stool test and of Clostridium difficile-derived toxin A/B in the feces, (b) intestinal permeability using the lactulose/mannitol (LA/MA) test, (c) frequent use of antibiotics due to recurrent infections during the first 2 years of postnatal life, and (d) stool habits with the Bristol Stool Form Scale. Chronic constipation was the only variable significantly associated with total urinary p-cresol concentration (P < 0.05). No association was found with presence of Clostridium spp. in the gut flora (P = 0.92), augmented intestinal permeability (P = 0.18), or frequent use of antibiotics in early infancy (P = 0.47). No ASD child was found to carry C. difficile in the gut or to release toxin A/B in the feces. In conclusion, urinary p-cresol levels are elevated in young ASD children with increased intestinal transit time and chronic constipation.
The aromatic compound p-cresol (4-methylphenol) has been found elevated in the urines of Italian autistic children up to 8 years of age. The present study aims at replicating these initial findings in an ethnically distinct sample and at extending them by measuring also the three components of urinary p-cresol, namely p-cresylsulfate, p-cresylglucuronate and free p-cresol. Total urinary p-cresol, p-cresylsulfate and p-cresylglucuronate were significantly elevated in 33 French autism spectrum disorder (ASD) cases compared with 33 sex- and age-matched controls (p50.05). This increase was limited to ASD children aged 8 years (p50.01), and not older (p ¼ 0.17). Urinary levels of p-cresol and p-cresylsulfate were associated with stereotypic, compulsive/repetitive behaviors (p50.05), although not with overall autism severity. These results confirm the elevation of urinary p-cresol in a sizable set of small autistic children and spur interest into biomarker roles for p-cresol and p-cresylsulfate in autism.
The present and previous results (Altieri et al., 2011), confirm that urinary amounts of the toxic compound p-cresol and of its derivatives, especially p-cresylsulfate, are significantly elevated in a sizable subgroup of small autistic children. These results were replicated in two case-control samples belonging to distinct ethnic groups, recruited in different geographical areas in Europe and screened at two independent clinical sites. Unbiased metabolomic and microbiomic approaches will have to define the degree of connection between elevated urinary p-cresol, skewed urinary metabolomic profiles and gut flora composition in our ASD patients. Clinical studies involving large cohorts will also be needed to conclusively define possible dose-dependent influences on the spectrum and severity of clinical signs and symptoms of ASD, as well as on endophenotypic subgroupings. Finally, perspective studies of high-risk infant siblings will be instrumental in determining the potential of urinary p-cresol and/or p-cresylsulfate as biological markers for an ASD diagnosis in small children and for predicting developmental trajectories

Figure 2. Total urinary p-cresol concentrations by age group, in 33 ASD patients (grey bars) and in 33 age-matched, sex-matched and ethnically matched controls (white bars). Data are presented as mean ± S.E.M. Numbers inside each column represent sample sizes. **p50.01 for global case-control contrasts in 22 pairs aged 3–8.
Background: Autism Spectrum Disorder (ASD) is a neurodevelopmental disorder characterized by deficits in social interaction/communication, stereotypic behaviors, restricted interests, and abnormal sensory-processing. Several studies have reported significantly elevated urinary and foecal levels of p-cresol in ASD children, an aromatic compound either of environmental origin or produced by specific gut bacterial strains.
Methods: Since p-cresol is a known uremic toxin, able to negatively affect multiple brain functions, the present study was undertaken to assess the effects of a single acute injection of low- or high-dose (1 or 10 mg/kg i.v. respectively) of p-cresol in behavioral and neurochemical phenotypes of BTBR mice, a reliable animal model of human ASD.
Results: P-cresol significantly increased anxiety-like behaviors and hyperactivity in the open field, in addition to producing stereotypic behaviors and loss of social preference in BTBR mice. Tissue levels of monoaminergic neurotransmitters and their metabolites unveiled significantly activated dopamine turnover in amygdala as well as in dorsal and ventral striatum after p-cresol administration; no effect was recorded in medial-prefrontal cortex and hippocampus.
Conclusion: Our study supports a gene x environment interaction model, whereby p-cresol, acting upon a susceptible genetic background, can acutely induce autism-like behaviors and produce abnormal dopamine metabolism in the reward circuitry.
Preliminary data point toward possible correlations between urinary p-cresol concentrations and ASD severity measured using the Childhood Autism Rating Scale (CARS) [12]. Multiple mechanisms could account for the negative influences of p-cresol on neural function, ranging from membrane depolarization and increased susceptibility to seizures [18], to decreased Na+-K+ ATPase activity [19], to blunted conversion of dopamine (DA) to norepinephrine (NE) due to inhibition of dopamine-β-hydroxylase [20].
This study demonstrates that acute p-cresol administration to an animal model of ASD induces behavioral abnormalities closely resembling core symptoms of ASD and comorbidities frequently observed in autistic individuals. These results underscore the importance of gene x environment interaction models, able to merge genetic predisposition and evidence-based environmental exposure to specific neurotoxic compounds into a unitary scenario. From a mechanistic standpoint, these results move the field beyond well-established paradigms in the autism literature, such as the imbalance between glutamate and GABA to explain insistence on sameness and the co-morbidity with epilepsy [62], or the role of 5-HT in reference to hyperserotonemia, disruption of circadian rhythmicity, neuroinflammation and neuronal excitability [63,64,65]. In a complementary view, they point toward critical dopaminergic roles in autistic symptoms as being relevant as stereotypic behaviors, hyperactivity, anxiety and motivational drive towards inanimate objects. Thirdly, urinary gut-derived neurotoxic compounds, such as p-cresol, could serve as useful ASD biomarkers, whose specificity now deserves to be assessed in samples of young non-autistic children affected with chronic constipation. Finally, the correction of chronic constipation and microbiota transfer therapy represent two reasonable and testable approaches, aimed at partly ameliorating autistic behaviors by reducing the absorption of neurotoxic compounds of environmental origin or derived from specific gut-bacterial strains [66]. Studies addressing the efficacy of these therapeutic approaches will largely benefit from parallel assessments of urinary biomarkers, such as p-cresol and other gut-derived compounds, in order to provide mechanistic insights into their effects on the longitudinal time course of autistic symptoms.
The paper below covers all kinds of issues and is a good read:
With the use of molecular techniques, numerous studies have evaluated the composition of the intestinal microbiota in health and disease. However, it is of major interest to supplement this with a functional analysis of the microbiota. In this review, the different approaches that have been used to characterize microbial metabolites, yielding information on the functional end products of microbial metabolism, have been summarized. To analyze colonic microbial metabolites, the most conventional way is by application of a hypothesis-driven targeted approach, through quantification of selected metabolites from carbohydrate (e.g., short-chain fatty acids) and protein fermentation (e.g., p-cresol, phenol, ammonia, or H2S), secondary bile acids, or colonic enzymes. The application of stable isotope-labeled substrates can provide an elegant solution to study these metabolic pathways in vivo. On the other hand, a top-down approach can be followed by applying metabolite fingerprinting techniques based on 1H-NMR or mass spectrometric analysis. Quantification of known metabolites and characterization of metabolite patterns in urine, breath, plasma, and fecal samples can reveal new pathways and give insight into physiological regulatory processes of the colonic microbiota. In addition, specific metabolic profiles can function as a diagnostic tool for the identification of several gastrointestinal diseases, such as ulcerative colitis and Crohn's disease. Nevertheless, future research will have to evaluate the relevance of associations between metabolites and different disease states.
Urinary levels of p-cresol and phenol have shown to be increased during high protein intake (37) and decreased after oral supplementation with oligofructose-enriched inulin (OF-IN) (25).


Pre- and/or probiotics can cause changes in the ecological balance of intestinal microbiota and hence influence microbial metabolic activities. In the present study, the influence of oligofructose-enriched inulin (OF-IN), Lactobacillus casei Shirota, and Bifidobacterium breve Yakult on the colonic fate of NH3 and p-cresol was investigated. A randomized, placebo-controlled, crossover study was performed in 20 healthy volunteers to evaluate the influence of short- and long-term administration of OF-IN, L. casei Shirota, B. breve Yakult, and the synbiotic L. casei Shirota + OF-IN. The lactose[15N,15N]ureide biomarker was used to study the colonic fate of NH3. Urine and fecal samples were analyzed for 15N content by combustion-isotope ratio mass spectrometery and for p-cresol content by gas chromatography-mass spectrometry. RT-PCR was applied to determine the levels of total bifidobacteria. Both short- and long-term administration of OF-IN resulted in significantly decreased urinary p-cresol and 15N content. The reduction of urinary 15N excretion after short-term OF-IN intake was accompanied by a significant increase in the 15N content of the fecal bacterial fraction. However, this effect was not observed after long-term OF-IN intake. In addition, RT-PCR results indicated a significant increase in total fecal bifidobacteria after long-term OF-IN intake. Long-term L. casei Shirota and B. breve Yakult intake showed a tendency to decrease urinary 15N excretion, whereas a significant decrease was noted in p-cresol excretion. In conclusion, dietary addition of OF-IN, L. casei Shirota, and B. breve Yakult results in a favorable effect on colonic NH3 and p-cresol metabolism, which, in the case of OF-IN, was accompanied by an increase in total fecal bifidobacteria.
Transitory Autism
Some people do grow out of their asthma, many people age out of their ADHD and some toddlers’ autism does fade away in early childhood.
I recall the developmental pediatrician who diagnosed my son at 3 years old, telling us that remarkable improvement up to the age of 6 does happen. That did not happen in our case.
Back in 2015, I highlighted a study from 2002 in Italy where Michele Zappella, an Italian doctor interested in autism and Tourette’s syndrome found that a subgroup of children diagnosed with autism and tics recover by the age of six.
Of course, nobody has bothered to find out why that might be.
We have a small new longitudinal study from UC Davis in Sacramento, which again shows how severity of autism can change from 3 years of age to 6 six years of age. Intervention made no difference, in spite of what Lovaas told us; so much for “evidence”.
Autism symptom severity change was evaluated during early childhood in 125 children diagnosed with autism spectrum disorder (ASD). Children were assessed at approximately 3 and 6 years of age for autism symptom severity, IQ and adaptive functioning. Each child was assigned a change score, representing the difference between ADOS Calibrated Severity Scores (CSS) at the two ages. A Decreased Severity Group (28.8%) decreased by 2 or more points; a Stable Severity Group (54.4%) changed by 1 point or less; and an Increased Severity Group (16.8%) increased by 2 or more points. Girls tended to decrease in severity more than boys and increase in severity less than boys. There was no clear relationship between intervention history and membership in the groups.

Scatterplot of individual ADOS CSS of all children in the sample at Time 1 and Time 3, by group membership. The DSG and SSG show a large range of individual severity scores at both Time 1 and Time 3 while The ISG shows a narrower range. Note, scores at Time 1 are plotted with jitter so that all individuals can be seen; participants plotted slightly below 4 actually received an ADOS CSS of 4
Optimal Outcome
A total of seven participants, 5.6% of the sample, had an ADOS CSS below the ASD cutoff at Time 3, thus potentially demonstrating optimal outcome. Six of these children were in the DSG (four girls and two boys) and one boy was in the SSG. These children had a mean severity level of 5 at Time 1 (range 4–7) and 1.8 at Time 3 (range 1–3). Their mean severity change was − 3.1 (range − 1 to − 6). All showed an increase in IQ over time, with IQ rising from a mean of 85.8 (range 75–95.8) to a mean of 105.3 (range 91–115). Adaptive functioning change (using the VABS-II composite score) was less consistent, as two children showed decreases and four showed increases over time (one child did not have a score at Time 1). Mean Time 1 adaptive function was 79.3 (range 71–92) and mean Time 3 was 89.6 (range 71–122).
Is Initial Autism Severity a Predictor of Severity Change?
For most children who were participants in this study, their autism symptom severity level at age 3 was not a good predictor of the severity change they underwent during early childhood.
Is Intervention History Associated with Differences in Severity Change?
The large majority of children in the Autism Phenome Project and GAIN study have received substantial amounts of intervention across childhood. Analysis of intervention history (total number of hours of intervention received and intensity of intervention) did not show significant differences between the groups.
Is IQ Associated with Differences in Severity Change?
IQ demonstrated a significant, negative relationship with symptom severity change; as IQ scores increased from age 3 to age 6, symptom severity levels decreased.
How is Adaptive Function Associated with Autism Severity Change?
Adaptive Functioning also demonstrated a significant, negative relationship with severity change. As symptom severity decreased from age 3 to age 6, adaptive functioning increased.
Optimal Outcome and Severity Change over Time
This study was initially motivated by the phenomenon of optimal outcome. Optimal outcome is traditionally defined as a decrease in autism symptoms in individuals previously diagnosed with ASD, so that they no longer meet diagnostic criteria (Fein et al. 2013). A total of seven participants, 5.6% of our sample, received an ADOS CSS below the ASD cutoff (1–3) at Time 3. Six of these children were in the DSG (four girls and two boys) and one boy was in the SSG. Since Optimal outcome is defined based on different aspects of function as well as autism symptom level (Fein et al. 2013), additional evaluations would have to be carried out concerning both the home and educational environments to confirm that these children have actually achieved optimal outcome.
Optimal outcome might also be interpreted more generally as indicating significant intra-individual change rather than the attainment of a specific cut-off score. This definition takes a wider approach to understanding the complex and variable ways in which children with autism grow and develop (Georgiades and Kasari 2018). If we apply this perspective to the current study’s results, the notion of optimal outcome would be relevant to many more children in the DSG who, while not decreasing below the ASD cut-off score, experienced substantial personal decrease in autism severity over time.
Why do some young children have “Transitory Autism”
It has long been known that some toddlers diagnosed with autism have very positive outcomes.
Our Developmental Pediatrician put it down to their brains being so plastic.
Other people think that autism is a hard-wired brain anomaly, fixed for good.
The reality is that you can both create and then reverse “autism” in many models of autism, so at least some types are not hard wired.
We saw how you can induce autism with propionic acid and then reverse those changes by taking the antioxidant NAC.
If you have a low fiber diet and lack healthy gut bacteria you will produce too much propionic acid, and not enough butyric acid.
People with autism who respond to Rifamixin may be among those who were suffering from too much propionic acid.
It does look like some people’s milder autism is in their gut and that some toddler’s severe autism is made even worse by what is going on in their colon.
Conclusion
Signs of any abnormal GI function should always be investigated in someone diagnosed with autism. Correcting dysbiosis (impaired microbiota/gut bacteria) should improve autism. Correcting deficiencies in diet should improve autism. Correcting GI inflammation should improve autism.
Dr Persico clearly would like there to be more testing of P-Cresol in urine, he sees it as a potential biomarker for autism.
Microbiota transplants are not widely on offer, but do appear to be a way to fix problems that you do not need to fully understand. How many other nasties like P-cresol are there in the autistic person’s gut? It is certainly conceivable that what therapy works for P-cresol will work for other nasties.
You would hope that all these Italian studies would lead up to a trial of oligofructose-enriched inulin or some probiotic bacteria to see if they can reduce both P-cresol in urine and the severity of autism (ADOS or CARS scales would be fine, Dr Persico).
You would hope that the in microbiota transplant trials in the US they are measuring what changes afterwards, hopefully they read Dr Persico’s research and measure P-Cresol and indeed the SCFAs propionic and butyric acid.
The UC Davis study again shows us that no single intervention is associated with the best outcomes in autism. The best outcomes just seem to "happen". They are not the result of any particular early intervention. That does not mean do nothing, it just means that mainstream autism interventions are not as potent as their advocates keep telling us. The billions of dollars spent on early intervention and ABA programs may not be the most effective allocation of resources.