Chamomile, a good source of Apigenin
Today we return to flavonoids, those
healthy chemicals found in fruits, vegetables, flowers etc.
In particular, the focus is on apigenin,
found in things like chamomile, parsley, oregano and in medicinal herbs like
Bacopa monnieri.
Why the interest
in Apigenin?
I did discover a while back that sound
sensitivity in some autism responds almost immediately to low dose Ponstan
(Mefenamic acid), which is a widely used as a pain reliever.
I was recently informed by a reader
who responds well to Ponstan (250mg once a day) that he gets exactly the same relief from sound sensitivity from taking
the flavonoid Apigenin (500mg a day).
Both Ponstan and Apigenin are OTC in
many countries. In countries like Greece Ponstan is extremely cheap. In the US Ponstan is very expensive and
supplements tend to be cheap.
For adults with sound sensitivity
drinking chamomile tea might be a good source of 50 mg of Apigenin (you would need
about 20g of chamomile flowers). Using the dried flowers likely gives better
results than ready-made tea bags.
Pleiotropic
effects
Both Ponstan and apigenin have
numerous beneficial effects. I noted in
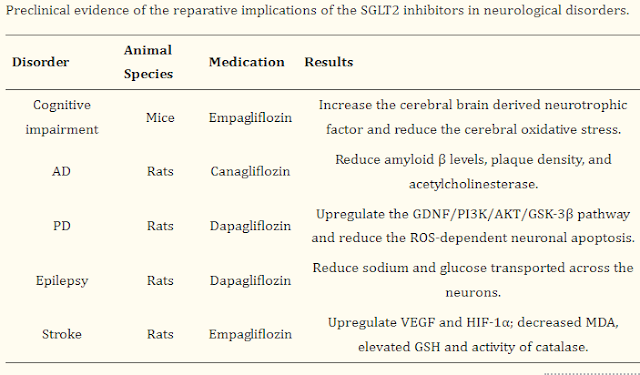
my earlier posts on Ponstan that it seems to offer protection from Alzheimer’s.
Perhaps surprisingly, people who take Ponstan are much less likely to develop
Alzheimer’s. Nobody has studied apigenin in human Alzheimer’s, but in animal
studies, apigenin has been shown to improve cognitive function, reduce amyloid
plaques, and protect neurons from damage.
Other Flavonoids
used in Autism
Dr Theoharides wrote a lot about
flavonoids to treat autism and mast cell disorders. His product Neuroprotek is a combination of
three flavonoids: luteolin, quercetin, and rutin, which are found in plants
such as celery, onions, and citrus fruits.
Epigallocatechin
gallate (EGCG) is a flavonoid found in green tea. The Spanish like doing
research on EGCG and they believe it has promise as an autism therapy. One of the
effects is to modify the gut microbiome. EGCG has also been shown to
accumulates in mitochondria making it an interesting therapeutic candidate for
neurodegenerative diseases involving neuronal apoptosis triggered by
mitochondrial oxidative stress. It has been studied in Down syndrome, Rett
syndrome and some other models of autism.
A very
detailed overview is available in the paper below:-
The
Emerging Role of Flavonoids in Autism Spectrum Disorder: A Systematic Review
Although autism spectrum disorder (ASD) is a
multifaceted neurodevelopmental syndrome, accumulating evidence indicates that
oxidative stress and inflammation are common features of ASD. Flavonoids, one
of the largest and best-investigated classes of plant-derived compounds, are
known to exert antioxidant, anti-inflammatory, and neuroprotective effects.
This review used a systematic search process to assess the available evidence
on the effect of flavonoids on ASD. A comprehensive literature search was
carried out in PubMed, Scopus, and Web of Science databases following the
PRISMA guidelines. A total of 17 preclinical studies and 4 clinical
investigations met our inclusion criteria and were included in the final
review. Most findings from animal studies suggest that treatment with
flavonoids improves oxidative stress parameters, reduces inflammatory
mediators, and promotes pro-neurogenic effects. These studies also showed that
flavonoids ameliorate the core symptoms of ASD, such as social deficits,
repetitive behavior, learning and memory impairments, and motor coordination.
However, there are no randomized placebo-controlled trials that support the
clinical efficacy of flavonoids in ASD. We only found open-label studies and
case reports/series, using only two flavonoids such as luteolin and quercetin.
These preliminary clinical studies indicate that flavonoid administration may
improve specific behavioral symptoms of ASD. Overall, this review is the first
one to systematically report evidence for the putative beneficial effects of
flavonoids on features of ASD. These promising preliminary results may provide
the rationale for future randomized controlled trials aimed at confirming these
outcomes.
It seems
that the many flavonoids have numerous beneficial effects - this is why it is
important to include them in your diet.
Sytrinol
Years ago, I wrote about Sytrinol, a
dietary supplement that is made from citrus peel extract. It contains
polymethoxylated flavones (PMFs), which are a type of flavonoid. It mainly contains
nobiletin and tangeritin, flavones that are found in citrus fruits, such as
lemons, oranges, and grapefruits. They have been shown to have a number of
health benefits, including lowering cholesterol, reducing inflammation, and
protecting cells from damage.
The idea was of interest because these
flavones are known to activate PPAR-gamma, which seemed potentially beneficial
in autism. Readers did confirm Sytrinol
provided a cognitive benefit, but it only lasts a few days and is then lost.
Sources of
Apigenin
Apigenin is sold as a supplement.
Chamomile
is one of the oldest, most widely used and well documented medicinal plants in
the world and has been recommended for a variety of healing applications for
centuries. Apigenin is thought to be one of the most potent substances found
within it.
Bacopa monnieri is another rich
source of flavonoids being a good source of luteolin and apigenin. An extract of Bacopa
monnieri, a nootropic herb, has been used to evaluate its neuroprotective
effect in a valproic acid (VPA) model of ASD. The results showed that B.
monnieri extract may attenuate VPA-induced damage by restoring antioxidant
enzymes and reducing inflammatory cytokines in the hippocampus and prefrontal
cortex.
The
biological effects of Apigenin
What does the Google AI (artificial intelligence) program Bard have to say:-
Apigenin is a flavonoid that is found in a variety of plants,
including chamomile, parsley, celery, and citrus fruits. It has several
potential health benefits, including:
Antioxidant. Apigenin is an antioxidant, which means it can help protect
cells from damage caused by free radicals. Free radicals are unstable molecules
that can damage DNA, proteins, and other cellular structures.
Anti-inflammatory. Apigenin has anti-inflammatory properties, which can help
reduce inflammation in the body. Inflammation is a contributing factor to many
diseases, including heart disease, cancer, and arthritis.
Cancer prevention. Apigenin has been shown to have cancer-fighting properties
in both animal and human studies. It may help prevent cancer by blocking the
growth and spread of cancer cells.
Brain health. Apigenin may be beneficial for brain health. It has been
shown to improve cognitive function in animal studies, and it may also help
protect against Alzheimer's disease and other neurodegenerative diseases.
Heart health. Apigenin may help improve heart health. It has been shown to
lower blood pressure and cholesterol levels, and it may also help protect
against heart arrhythmias.
Hormone modulation. Apigenin may modulate the production of hormones, such as
estrogen and testosterone. This could have benefits for women's health, such as
reducing the risk of breast cancer and improving menopausal symptoms.
Immune health. Apigenin may boost the immune system. It has been shown to
increase the production of white blood cells, which help fight infection.
Other benefits. Apigenin may also have other health benefits, such as
relieving anxiety, promoting sleep, and strengthening bones.
When you push Bard a little bit you get more:
Apigenin
and ion channels, Bard?
Apigenin is a flavonoid that has been shown to interact with
a variety of ion channels in the body. These include:
Voltage-gated calcium channels. Apigenin has been shown to inhibit
the activity of voltage-gated calcium channels, which are involved in the
regulation of many cellular processes, including muscle contraction, cell
growth, and cell death.
Transient receptor potential vanilloid 4 (TRPV4) channels. TRPV4 channels are activated by
heat and inflammation, and they play a role in pain perception,
thermoregulation, and inflammation. Apigenin has been shown to activate TRPV4
channels, which could have potential implications for the treatment of pain and
inflammation.
Nicotinic acetylcholine receptors (nAChRs). nAChRs are ligand-gated ion channels
that are activated by acetylcholine. They are involved in a variety of
functions, including learning, memory, and muscle contraction. Apigenin has
been shown to potentiate the activity of nAChRs, which could have potential
implications for the treatment of Alzheimer's disease and other
neurodegenerative diseases.
Potassium channels: Potassium channels are responsible for the efflux of
potassium ions from cells. Apigenin has been shown to activate some types of
potassium channels, which can have cardioprotective effects.
Gamma-aminobutyric acid (GABA)A receptors. GABAA receptors are ligand-gated
ion channels that are activated by GABA. They are involved in the regulation of
anxiety, sleep, and epilepsy. Apigenin has been shown to modulate the activity
of GABAA receptors, which could have potential implications for the treatment
of anxiety and epilepsy.
Which potassium channels, Bard?
Apigenin has been shown to activate some types of potassium
channels, including:
Small conductance calcium-activated potassium channels (SK
channels): SK channels are activated by calcium ions and play a role in
regulating cell excitability. Apigenin has been shown to activate SK channels
in a number of cell types, including neurons, smooth muscle cells, and cardiac
cells.
Large conductance calcium-activated potassium channels (BK
channels): BK channels are also activated by calcium ions and play a role in
regulating cell excitability and blood pressure. Apigenin has been shown to
activate BK channels in some cell types, but the effects are less well-studied
than the effects on SK channels.
Transient receptor potential vanilloid 4 (TRPV4) channels:
TRPV4 channels are activated by a variety of stimuli, including heat,
inflammation, and mechanical stress. Apigenin has been shown to activate TRPV4
channels in some cell types, but the effects are less well-studied than the
effects on SK and BK channels.
The effect of mefenamic acid on potassium channels, Bard?
Mefenamic acid has been shown to have effects on a variety of
ion channels, including potassium channels.
In vitro studies have shown that mefenamic acid can activate
certain types of potassium channels, such as small conductance
calcium-activated potassium channels (SK channels) and large conductance
calcium-activated potassium channels (BK channels). This activation of potassium channels can lead to
a decrease in the excitability of cells, which can be beneficial in conditions
where excessive cell excitability is a problem, such as epilepsy and
arrhythmias.
However, mefenamic acid can also inhibit certain types of potassium channels, such as ATP-sensitive potassium channels (KATP channels). This inhibition of KATP channels can lead to an increase in the excitability of cells, which can be harmful in conditions where excessive cell excitability is a problem, such as heart arrhythmias.
The effects of mefenamic acid on potassium channels are
complex and depend on the type of channel, the concentration of mefenamic acid,
and the cell type. More research is needed to fully understand the mechanisms
by which mefenamic acid interacts with potassium channels and the implications
for its potential therapeutic applications.
Apigenin
in Down syndrome
Plant Compound Apigenin Reduces Cognitive Deficits in Mouse Model of Down Syndrome
Mice treated with
apigenin had better memory and developmental milestone scores.
The plant compound apigenin improved the cognitive and memory deficits usually seen in a
mouse model of Down syndrome, according to a study by researchers at the
National Institutes of Health and other institutions.
Apigenin is found in chamomile flowers, parsley, celery,
peppermint, and citrus fruits. The researchers fed the compound to pregnant
mice carrying fetuses with Down syndrome characteristics and then to the
animals after they were born and as they matured.
The findings raise the
possibility that a treatment to lessen the cognitive deficits seen in Down
syndrome could one day be offered to pregnant women whose fetuses have been
diagnosed with Down syndrome through prenatal testing. The study appears in the American
Journal of Human Genetics.
Down syndrome is a set of symptoms resulting from an extra
copy or piece of chromosome 21. The intellectual and developmental disabilities
accompanying the condition are believed to result from decreased brain growth
caused by increased inflammation in the fetal brain.
Apigenin is not known to have any toxic effects, and previous
studies have indicated that it is an antioxidant that reduces inflammation. Unlike many compounds, it is
absorbed through the placenta and the blood brain barrier, the cellular layer
that prevents potentially harmful substances from entering the brain.
Compared to mice with Down symptoms whose mothers were not
fed apigenin, those exposed to the compound showed improvements in tests of
developmental milestones and had improvements in spatial and olfactory memory. Tests of gene activity and
protein levels showed the apigenin-treated mice had less inflammation and
increased blood vessel and nervous system growth.
Human fetuses with trisomy 21 (T21) have atypical brain development that is apparent sonographically in the second trimester. We hypothesize that by analyzing and integrating dysregulated gene expression and pathways common to humans with Down syndrome (DS) and mouse models we can discover novel targets for prenatal therapy. Here, we tested the safety and efficacy of apigenin, identified with this approach, in both human amniocytes from fetuses with T21 and in the Ts1Cje mouse model. In vitro, T21 cells cultured with apigenin had significantly reduced oxidative stress and improved antioxidant defense response. In vivo, apigenin treatment mixed with chow was administered prenatally to the dams and fed to the pups over their lifetimes. There was no significant increase in birth defects or pup deaths resulting from prenatal apigenin treatment. Apigenin significantly improved several developmental milestones and spatial olfactory memory in Ts1Cje neonates. In addition, we noted sex-specific effects on exploratory behavior and long-term hippocampal memory in adult mice, and males showed significantly more improvement than females. We demonstrated that the therapeutic effects of apigenin are pleiotropic, resulting in decreased oxidative stress, activation of pro-proliferative and pro-neurogenic genes (KI67, Nestin, Sox2, and PAX6), reduction of the pro-inflammatory cytokines INFG, IL1A, and IL12P70 through the inhibition of NFκB signaling, increase of the anti-inflammatory cytokines IL10 and IL12P40, and increased expression of the angiogenic and neurotrophic factors VEGFA and IL7. These studies provide proof of principle that apigenin has multiple therapeutic targets in preclinical models of DS.
Conclusion
I am
still delighted to have found a treatment for my son’s sound sensitivity, which got much more extreme almost overnight a couple of years ago.
I had
already established long ago that he got short term sound sensitivity relief from taking a
potassium supplement. Some readers found
a potassium supplement provided long term relief.
I
thought that Ponstan might provide a good longer term solution and indeed it worked from
the first pill. This low dose therapy
also works for other people with sound sensitivity, even one adult who has no
autism. The effective adult dose is 250
mg once a day.
Unlike
other fenamate class drugs, like Diclofenac, Ponstan seems to be free from GI side
effects at this low dose in most people.
Apigenin
is an interesting alternative for those who do not tolerate Ponstan well, or
who cannot access it.
A common
link between what seems to improve sound sensitivity:
•
Oral potassium
•
Ponstan (Mefenamic acid)
•
Apigenin
is potassium ion channels.
If you
ask Google’s AI program Bard, he will tell you:
“It is possible that all 3 substances could
affect the same potassium ion channel in some cell types, but this has not been
definitively shown. More research is needed to fully understand the effects of
these substances on potassium ion channels.”
Technically Bard is genderless, but he is a reflection of the programmers behind the software. In our house he is called Bart anyway.
Bart
does make mistakes, contradicts himself in the same answer and he gives you different answers if you ask the same question
more than once. He is also prone to mixing things up, just like humans do.